- The findings and conclusions described in this article are those
of the author and do not necessarily represent the views of the
Centers for Disease Control and Prevention. - On September 22, 2006 the Centers for Disease Control and Prevention (CDC) published recommendations for a major change in the approach to testing for HIV infection in the United States: expanded screening in healthcare settings with streamlined procedures for consent and pretest information,[1] available at http://www.cdc.gov/mmwr/PDF/rr/rr5514.pdf. The CDC's specific recommendations for healthcare settings, outlined in Table 1, included:
- expanded HIV screening for patients regardless of risk;
revisions to procedures for separate, written informed consent;
indications for diagnostic testing; and
decreased emphasis on prevention counseling. Table 1. Summary: CDC Recommendations for HIV Testing of Adults and Adolescents in Healthcare Settings| Screening | | All persons aged 13-64, regardless of risk, should receive routine, voluntary screening for HIV in all healthcare settings in which the prevalence of undiagnosed HIV infection is at least 0.1%. | | All patients initiating treatment for TB should be screened for HIV. | | All patients seeking treatment for STDs should be screened for HIV each time they seek such treatment. | | Healthcare providers should encourage patients and their prospective sex partners to be tested before initiating a new sexual relationship. | | Repeat HIV screening should be performed for patients with known risk at least annually. | | Persons likely to be at high risk include injection-drug users and their sex partners, persons who exchange sex for money or drugs, sex partners of HIV-infected persons, and men who have sex with men (MSM) or heterosexual persons who themselves or whose sex partners have had more than one sex partner since their most recent HIV test. |
- This type of screening, known as opt-out testing, is carried out after notifying the patient that an HIV test will be performed and that the patient may elect to decline or defer testing. Thus, consent is inferred unless the patient declines testing. Opt-out testing is sometimes referred to as "routine testing," but the two are not synonymous. In opt-out testing, patients are notified that an HIV test is a routine part of the encounter and as such there is no requirement for formalized counseling or separate written informed consent. Patients must specifically decline testing, either orally or in writing, to be exempt from having an HIV test. Routine testing, on the other hand, is the routine offer of an HIV test, followed by whatever protocol is required in that setting or state.
Rationale for the CDC's Revised Recommendations- The impetus for the revised recommendations came from several observations. First, effective treatment with highly active antiretroviral therapy (HAART) has substantially changed the risk-benefit ratio associated with HIV testing, transforming AIDS from a fatal disease to a highly treatable chronic condition: A 25-year-old, HIV-infected person who is receiving care in the 21st century can expect to live another 38.9 years, only 12 years less than the estimated life expectancy of an uninfected counterpart.[2]Second, persons who know they are infected with HIV are 3.5 times less likely to transmit HIV to uninfected partners than persons unaware of their infection.[3] Thus, increasing the number of HIV-infected persons who know they are infected could lead to a considerable reduction in new infections. Third, technical advances in testing methods (including rapid HIV tests) have made HIV testing more feasible in a variety of healthcare venues.[4] Finally, efforts focused on changing behavior in the large, uninfected population have been insufficient to stem the spread of HIV. More than 1 million Americans are estimated to be living with HIV, nearly a quarter of whom remain undiagnosed,[5] and at least 40,000 new infections occur each year.
The Critical Role of Nursing- Of the demonstration projects designed to explore alternative models for HIV screening, those that are nursing-driven have proven most effective. Using existing nursing staff to obtain consent, provide pre- and post-test information, and perform point-of-care HIV testing has several advantages over using supplemental HIV counseling and testing staff to provide these services. First, it allows HIV testing to be offered 24 hours a day, 7 days per week without hiring additional personnel. In comparison studies,[6] a nursing-driven program allowed many more HIV tests to be performed than in programs with a limited number of supplemental staff dedicated to conducting HIV counseling and testing. In 15 months, nurses were able to test nearly 6400 patients and identify 65 new HIV infections in an Oakland emergency department (ED). During the same time period, counselor-based models tested 1700 patients and found 13 new HIV infections in a comparable Los Angeles ED; and in New York, supplemental staff was able to test only 1300 patients and discover 19 patients with previously-undiagnosed HIV infection.
Late Diagnosis of HIV and Implications for Survival- Several studies now document that many HIV-infected patients make numerous healthcare visits in acute care, managed care, and primary care settings but are not tested for HIV until late in the course of their disease -- too late to derive optimal benefit from antiretroviral therapy.[7-9] Data from domestic HIV surveillance consistently indicate that 40% of patients receive an AIDS diagnosis within 1 year of their first positive HIV test. Taking into account the natural history of HIV infection, this means that an average of 7 to 9 years elapse before diagnosis for these late testers, during which they may unknowingly transmit HIV and fail to receive effective therapy. Earlier diagnosis and therapy confer distinct survival advantages. Mean survival when HIV is detected with a CD4 count of 320/mcL is estimated to be 24.2 years, compared with 13 years when treatment is initiated at a CD4 count of 87/mcL. Median survival after AIDS diagnosis has increased from 1.6 years in the absence of treatment to 14.9 years in the era of HAART.[10]
Diagnostic Testing vs Opt-out Screening- To be sure, diagnostic testing for HIV infection, especially acute HIV infection, remains a stalwart of good clinical care. The CDC recommendations regarding such diagnostic testing are shown in Table 2.
Table 2. Summary: CDC Recommendations for HIV Testing of Adults and Adolescents in Healthcare Settings| Diagnostic Testing | | All patients with signs or symptoms consistent with HIV infection or an opportunistic illness characteristic of AIDS should be tested for HIV. | | Clinicians should maintain a high level of suspicion for acute HIV infection in all patients who have a compatible clinical syndrome and who report recent high-risk behavior. | | When acute retroviral infection is a possibility, an RNA test should be performed in conjunction with an HIV antibody test. |
- Further, as shown in Table 3, healthcare settings -- doctors' offices, hospitals, emergency departments, and community clinics -- account for more than 75% of the estimated 16-22 million HIV tests performed annually in the United States, and for nearly two thirds of all HIV diagnoses.[11]
Table 3. Source of HIV Tests and Positive Tests, United States, 2002
| HIV Tests* | HIV+ Tests** |
|---|
| Private doctor/HMO | 44% | 17% | | Hospital, ED, Outpatient | 22% | 27% | | Community clinic (public) | 9% | 21% | | HIV counseling/testing | 5% | 9% | | Correctional facility | 0.6% | 5% | | STD clinic | 0.1% | 6% | | Drug treatment clinic | 0.7% | 2% |
Sources: * National Health Interview Survey, 2002;[11] **Supplement to HIV/AIDS Surveillance, 2000-2003, CDC unpublished data - Because HIV testing has traditionally been based on risk (either explicitly or implicitly), clinicians often do not consider the diagnosis of HIV infection until patients present with symptoms of immunodeficiency. As seen in the Figure, those tested less than 1 year before an AIDS diagnosis do so much more commonly because of illness than those who are diagnosed earlier in the course of HIV infection. Late testers, compared with those tested early, tend more often to be younger, heterosexual, less educated, and African American or Hispanic.[11]
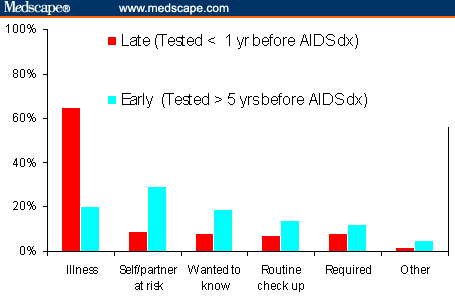 Figure. Percentage of late and early testers, by reason for testing -- 16 sites, US 2000-2003.
Source: CDC. Late versus early testing of HIV -- 16 sites, United States, 2000-2003. MMWR. 2003;52:581-586. - Of the 40,000 persons who acquire HIV infection each year, an estimated 40% to will experience symptoms of acute HIV infection,[12-14] and 50% to 90% of these patients will seek medical care. In general, patients present with the symptoms of viral illness shown in Table 4 and, of those diagnosed with acute HIV, 50% of patients are seen at least 3 times before the diagnosis of acute HIV infection is established.
Table 4. Clinical Manifestations of Acute HIV Infection, 101 Seroconverters, HIVNET Cohort, 1995-98| Symptom | Percentage | Median Duration
Days (IQR) |
|---|
| Any symptom | 85% |
| | Fatigue | 56% | 9 (5-29) | | Fever | 55% | 5 (4-10) | | Pharyngitis | 43% | 7 (5-10) | | Lymphadenopathy | 36% | 7 (4-14) | | Rash | 16% | 8 (6-14) |
Source: Celum CL, et al.[13] - One study, based on national ambulatory medical care surveys, estimated that the prevalence of acute HIV infection was 0.5% to 0.7% among ambulatory patients who sought care for fever or rash.[15] In persons with a negative or indeterminate HIV antibody test, acute HIV infection can be diagnosed by detecting HIV RNA in plasma. Although the long-term benefit of HAART during acute HIV infection has not been established conclusively,[16] identifying primary HIV infection can reduce the spread of HIV that might otherwise occur during the acute phase of HIV disease.
Advances in HIV Testing Technology- Techniques for detecting HIV infection are now substantially easier and less expensive, with a more rapid turnaround time for test results. Conventional testing, the enzyme immunoassay screening test followed by a confirmatory Western blot, required the resources of a high-complexity laboratory and several days or weeks for completion. Because of the lag between initiation of testing and the availability of results, up to one-third of HIV-infected patients never received their test results. Since 2002, 6 rapid HIV tests have been approved by the Food and Drug Administration, including 4 commercial products that are CLIA-waived, require only saliva or a drop of blood with no specialized equipment, and yield results in 10-20 minutes with a sensitivity of 99.6% to 100% and a specificity of 99.7% to 100%.[4] A positive test result still requires confirmation, but a negative test is regarded as conclusive. Thus, for practical purposes, a rapid HIV test can be done in virtually any medical or non-medical setting and provide preliminary results at the time of testing with low cost and high accuracy. The CDC's recent recommendations regarding test results are shown in Table 5. The CDC Web page on rapid HIV testing is quite useful and includes descriptions of the rapid HIV tests approved by the FDA, how the tests can be implemented in different settings, and research on the effectiveness and possible uses of the tests; this information can be found at http://www.cdc.gov/hiv/rapid_testing.
Table 5. Summary: CDC Recommendations for HIV Testing of Adults and Adolescents in Healthcare Settings| Test Results | | HIV test results should be provided to patients in the same manner as results of other diagnostic or screening tests. | | HIV test results should be provided confidentially and by personal contact. | | HIV test results may be provided by telephone. | | Positive or negative HIV test results should be documented in the patient's confidential medical record and should be readily available to all healthcare providers involved in the patient's clinical management. |
Cost-Effectiveness- Analyses of costs and effectiveness concluded that expanded HIV screening is as cost-effective as other routinely recommended interventions (such as mammography and PAP testing) when the prevalence of HIV exceeds 0.1%.[17,18] The CDC recommends screening in all healthcare settings where HIV prevalence exceeds this 0.1% threshold. Because most clinicians do not know the prevalence of undiagnosed HIV infection in their practice setting, they should initiate screening to determine its potential yield. If screening identifies less than 1 new infection per 1000 patients screened, continued universal screening is not warranted; targeted screening for patients at increased risk for HIV should be conducted.
Prevention Counseling- Counseling with testing has been a longstanding HIV prevention strategy, but studies have not demonstrated whether it reduces the rate of HIV acquisition. A meta-analysis of 27 studies found that HIV-negative persons failed to modify behavior as a result of counseling with HIV testing.[19] However, patients at 4 sexually transmitted disease (STD) clinics who received theory-based, carefully structured prevention counseling from well-trained counselors showed an increase in condom use and a 30% decrease in the incidence of STDs at 6 months; a 20% decrease was still evident after 12 months.[20] In practice, this presents a paradox: counseling is viewed as potentially beneficial for disease prevention, but the need to provide counseling is also cited by providers as a major barrier to HIV testing,[21][22] The CDC's recent recommendations regarding pretest information, counseling, and consent in healthcare settings, shown in Table 6, do not advise against counseling, but presume that clinicians will use their judgment to provide or refer patients for counseling, when appropriate, as they would with any clinical test. and scarce financial and human resources often make intensive prevention counseling impractical.
Table 6. Summary: CDC Recommendations for HIV Testing of Adults and Adolescents in Healthcare Settings| Pretest Information, Counseling and Consent | | Screening should be voluntary, and should never be performed without the patient's knowledge and understanding that an HIV test will be performed. | | Patients should be informed orally or in writing that HIV testing will be performed unless they decline (opt-out screening). | | Providers should discuss and address reasons for declining an HIV test. | | HIV testing need not be linked explicitly to prevention counseling. | | Prevention counseling should not be required with HIV diagnostic testing or as part of HIV screening programs in healthcare settings. | | Prevention counseling is desirable for all patients at risk for HIV infection, but might not be appropriate or feasible in all settings. | | Prevention counseling is strongly encouraged for persons at high risk for HIV in settings in which risk behaviors are assessed routinely (eg, STD clinics) but should not pose a barrier to HIV testing. | | Consent for HIV screening should be incorporated into the patient's general informed consent for medical care on the same basis as other screening or diagnostic tests. | | Separate, signed consent forms for HIV testing are not recommended. | | If a patient declines the HIV test, this decision should be documented in the medical record. |
Evidence for Adoption of the Revised Recommendations- Initial reports from 33 projects presented in abstract form at the December 2007 National HIV Prevention Conference and the February 2008 Conference on Retroviruses and Opportunistic Infections show promising results. As shown in Table 7, 249,374 persons were tested, of whom 2,867 (1.2%) were newly diagnosed with HIV infection. The proportion of patients who tested positive varied considerably across different settings.
Table 7. Initial Results from HIV Screening Programs in Healthcare Settings| Setting | Number of Projects | Total Tested | Total Positive | % Positive | Median (range)
% positive |
|---|
| Emergency Departments | 13 | 64,217 | 629 | 0.98% | 1.04% (0.27-1.79) | | Primary Care | 5 | 7233 | 22 | 0.30% | 0.17% (0.05-0.95) | | Mixed Venues | 5 | 58,190 | 926 | 1.59% | 1.95% (0-6.02) | | Hospital/Ambulatory | 4 | 103,233 | 963 | 0.93% | 1.35% (0.34-3.67) | | HIV/STD Clinics | 4 | 5634 | 85 | 1.51% | 4.61% (0.39-11.41) | | Prisons | 4 | 10,279 | 219 | 2.13% | 0.95% (0-3.63) | | Mental Health Clinic | 1 | 588 | 23 | 3.91% |
| | Total |
| 249,374 | 2867 | 1.15% | 0.95% (0-11.41) |
- At the time the CDC's recommendations were issued, laws in numerous states required signed informed consent for HIV testing, and pre- or post-test counseling, or both.[23] Many of these laws, established at a time when no effective therapy for HIV infection existed and when those who tested positive faced an extraordinary fear of contagion, are less relevant now that therapy has become increasingly effective and the stigma associated with HIV infection has been substantially reduced (although not eliminated).[24] Since the recommendations were issued, legislation to remove barriers to opt-out testing has been passed in 14 states (California, Georgia, Illinois, Indiana, Iowa, Louisiana, Maine, Nevada, New Hampshire, New Jersey, New Mexico, North Carolina, Rhode Island, and Tennessee)[25] and introduced in 7 others. Several states (eg, Florida and Missouri) have reviewed their state regulations and found no impediments to adopting the recommendations. An updated compendium of state-by-state testing laws can be accessed at: http://www.ucsf.edu/hivcntr/StateLaws/Index.html
- The 2006 CDC Revised Recommendations provide an opportunity to accelerate domestic HIV prevention efforts through increasing the proportion of individuals who know their HIV status and promoting earlier access to effective treatment. Changing clinical attitudes and practice will be incremental but rewarding, requiring sustained leadership at all levels of society.
- This activity is supported by an independent educational grant from Gilead.
- References
 Contents of: Expanded HIV Testing -- Implementing the CDC Recommendations: Guidance for Nurses All sections of this activity are required for credit. - Expanded HIV Testing in Nursing Care: Implementing the CDC RecommendationsDr. Bernard M. Branson discusses the rationale for the CDC guidelines on expanded HIV testing and outlines strategies for their implementation by nurses.Bernard M. Branson, MD (Clinical Update, March 28, 2008)
- HIV Opt-out Testing: The Role of the Nurse: An Expert Interview With Carl Kirton and Lyn C. StevensNurses are often the professionals called upon to make things happen in clinical settings. Learn from these HIV nurse-experts about how to implement an HIV opt-out testing program.Lyn C. Stevens, MS, NP, ACRN; Carl A. Kirton, MA, RN, ACRN, ANP-BC (Expert Interview, March 28, 2008)
- Implementing a Rapid HIV Testing Program in the Acute Care Setting: Nurses Take the LeadWould you know where to begin if you were charged with implementing an opt-out HIV testing program in a hospital setting? This case illustrates an approach that works.Carl A. Kirton, MA, RN, ACRN, ANP-BC; Lyn C. Stevens, MS, NP, ACRN (Test and Teach Case, March 28, 2008)
|







Tidak ada komentar:
Posting Komentar